The Renal System
- Christie Roberts
- Oct 15, 2020
- 9 min read
Updated: Jul 2, 2025
This post is going to take you on a whistle-stop tour of the structure and function of kidneys. It will also touch on AKI and CKD, which are explained further here.
The vast majority of people have 2 kidneys located posteriorly on either side of the spine. In normal anatomy, they are 10-15cm long and shaped like beans.
STRUCTURE OF THE KIDNEY
GROSS STRUCTURE
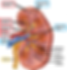
The kidney is com[prised of the cortex (outer layer) and medulla (inner layer). The nephrons (see below) are found in the outer cortex with tubules extending into the medulla.
The medulla contains 8-15 renal pyramids, which convene at a minor calyx. Several minor calyces combine to form a major calyx, and several major calyces will empty urine into the renal pelvis for urine to enter the ureter.
Each kidney has a suprarenal (adrenal) gland sitting on top of it like a hat. These glands are responsible for secretion of hormones including catecholamines, aldosterone and cortisol.
The main blood flow to the kidneys comes from the renal artery, which divides down into branches of segmental, interlobar, arcuate and interlobular arteries, which divide again into the afferent and efferent arterioles of the glomerulus (see below) and tiny peritubular capillaries providing blood flow to the nephrons. These then grow again until they turn into the renal vein, which takes the deoxygenated and filtered blood back to the heart and lungs,
FINE STRUCTURE- nephrons
The nephron is the functional unit of the kidney- the room where it happens. 'It' being filtration of blood and plasma to remove toxins (urea, creatinine), balance fluids and electrolytes (mostly sodium and potassium), and create urine. There are approximately 1.25 million nephrons in each kidney, and the presence of looping tubules increases the surface area available for diffusion.

Blood enters the glomerulus via the afferent arteriole. Here, hydrostatic pressure across the Bowman's Capsule forces small molecules such as water, glucose and electrolytes from the blood into the tubule across the semi-permeable membrane. Cells (such as RBCs) are too large to pass across the membrane, and only proteins smaller than albumin are able to cross (this is why presence of blood in urine- haematuria- or protein in urine- proteinuria- can be indicators of damage).
The filtrate continues through the nephron- the Proximal Convoluted Tubule (PCT), Loop of Henle, and the Distal Convoluted Tubule (DCT). Each section of the renal tubule is responsible for different aspects of filtration, as explained below. Filtered blood leaves via the efferent arteriole and continues around the capillary network surrounding each nephron, for reabsorption of certain molecules from the filtrate as it moves through the nephron. At the terminal end, there is a collecting duct which finalises the concentration and pH of the filtrate before it moves through the minor calyces, major calyces and renal pelvis to be excreted as urine.
FUNCTIONS OF THE KIDNEY
FILTRATION OF BLOOD and PRODUCTION OF URINE
Probably the best known function, your kidneys are responsible for filtering nitrogenous waste products like urea and creatinine from the blood, and balancing fluid and electrolytes, to create urine that helps to maintain homeostasis in the body.
Secretion and reabsorption occurs via diffusion and osmosis as blood moves round the nephron. A highly vascular capillary network, and convoluted tubule gives a large surface area, with the greatest concentration gradients possible to maximise the efficiency of filtration.
There are 4 stages to filtration in the nephron-
1. Glomerular filtration.
Here, blood enters the glomerulus via the afferent arteriole. Water and small solutes are forced through the fenestrated, semi permeable capillary walls as a result of hydrostatic and osmotic pressures, which influence the GFR- glomerular filtration rate. GFR is proportional to urine production (a higher GFR will lead to high urine formation). The resulting cell and protein free filtrate moves through the nephron, and filtered blood leaves the glomerulus via the efferent arteriole, which continues to loop around the tubule of the nephron ready for....
2. Tubular reabsorption.
This is a selective trans-epithelial process, where transport occurs both passively and actively. The molecules reabsorbed from filtrate back into the blood depends on the area of the nephron-

Across the nephron, the majority of molecules filtered out are reclaimed- practically 100% of organic nutrients, like amino acids and glucose are reabsorbed (unless glucose is so high that all glucose transporters are occupied, which lets some spill over into the urine and indicates a diabetes-sized problem...) while reabsorption of water and ions is variable dependent on bodily needs and hormone signals.
3. Tubular secretion.
Here, there is selective movement of substances from the blood into the filtrate to be excreted in urine. The PCT is the main site of secretion for basically everything, although other areas do also play a part. Molecules moved include nitrogenous waste products from the blood (urea, creatinine, ammonia), and also molecules produced in the tubular cells such as HCO3- (this contributes to pH maintenance- more on that later)

4. Water reabsorption.
This occurs by 2 different mechanisms of osmosis- reabsorption in the PCT is driven by the shifting osmolarity of blood around the nephron as a result of solute (namely Na+) reabsorption. The general rule is that where sodium goes, water will follow, through aquaporin membrane proteins. In the PCT, the presence of aquaporins 'obliges' the body to reabsorb water regardless of the state of hydration- this is obligatory water reabsorption. In the collecting duct, water movement is instead controlled by ADH. Aquaporins are absent unless ADH is present. This is facultative water reabsorption.
A note on ADH- aka vasopressin. It is made by the hypothalamus and stored/released by the posterior pituitary. It is stored or secreted in response to plasma osmotic pressure and fluid volume status, and is inhibited by ANP (which is released by stretched atria in response to high blood pressure). It does what it says on the tin- when released, it is an anti-diuretic- so it inhibits urine formation. This is to allow the body to retain more water.

Finally...
The end product after these 4 steps is urine, which consists of anything not reabsorbed, plus anything secreted. The volume and concentration depends on hormone levels, blood pressure and fluid balance.
In order to maintain the osmolarity of plasma around 300mOsm (this is important to prevent shrinking or swelling of cells- particularly in the brain), and to keep fluid balance in a normal range, the body will produce larger amounts of dilute urine if overhydrated (down to 100mOsm/L) and a smaller amount of concentrated urine if dehydrated (up to 1200mOsm/L).
Urine production can be summed up by:
Excretion = Filtration - Reabsorption + Secretion
Some terminology related to urine output-
Oliguria- low urine output
Anuria- no urine output
Polyuria- high urine output
Dysuria- painful or uncomfortable urine output
pH REGULATION
pH in the body is renally maintained through a balance of bicarbonate (HCO3-) and H+ ions. Normal pH is 7.35-7.45 when PCO2 is 4.5-6.0kPa and HCO3- is 22-26mmol/L. Both of these can be measured on an arterial blood gas. The kidneys are responsible for the metabolic regulation of pH through HCO3- (as opposed to the respiratory side, which is controlled by the lungs- for now, we're focusing on the renal side of things). If the pH goes out of equilibrium, the body will compensate to return it to a normal range- renally this means either retaining or excreting more or less HCO3- and H+. HCO3- is made by cells in the PCT and collecting ducts, and fine tuning of excretion/reabsorption to regulate pH occurs in the collecting duct.
In response to an acidosis (where bicarb and pH are low)- the renal tubule cells will secrete more H+ into urine, and reabsorb or produce more HCO3-. This leads the blood pH to increase.
In response to alkalosis (where bicarb and pH are high)- Cl- is reabsorbed instead of HCO3-, leading bicarb to be excreted in urine. This leads the blood pH to decrease.
BLOOD PRESSURE
Blood pressure will not only be affected by the fluid balance controlled by the kidneys, but also hormonal control with ADH and the Renin Angiotensin Aldosterone System (RAAS).
ADH- Osmoreceptors in the hypothalamus detect an increase in plasma osmolarity, a reduction in volume and a decrease in BP. Alongside baroreceptors in the atria and carotid arch, this stimulates the pituitary to release ADH. This targets the collecting ducts and inserts aquaporins to allow for more water reabsorption to improve plasma volume, osmolarity and BP. A small amount of concentrated urine is produced, and a negative feedback loop inhibits osmoreceptors and baroreceptors when BP rises. Stimulation of these receptors is also creates a sensation of thirst by the hypothalamic thirst centre.
RAAS- (there is a full post on RAAS here) In response to a drop in BP, decrease in GFR, and increase in plasma osmolarity, baroreceptor cells stimulate renal sympathetic nerve activity, and macula densa cells in the Loop of Henle stimulate juxtaglomerular granular cells near the DCT to release renin. Renin converts angiotensinogen from the liver into angiotensin I. Angiotensin I is converted into angiotensin II by ACE in the lungs. Angiotensin II stimulates the adrenal cortex to release aldosterone- a hormone responsible for enhancing reabsorption of sodium in the kidney (this leads to increased reabsorption of water, as water will follow sodium into the blood). Angiotensin II will also stimulate ADH release, activate the hypothalamic thirst centre, and lead to increased peripheral resistance through vasoconstriction.

VITAMIN D AND CALCIUM
Vitamin D and calcium are heavily linked, and the kidneys are responsible for both management of calcium absorption and activation of vitamin D.
Cholecalciferol (vitamin D3) and Ergocalciferol (vitamin D2) are inactive forms of Vit D absorbed from food or produced by the skin when exposed to sunlight- which is why nearly all of us become vitamin D deficient in the wintertime :(
Cholecalciferol is converted by the liver to calcifediol, which is then further converted by the kidneys into calcitriol.- which aids in calcium absorption
Calcium is reabsorbed in the DCT through action of parathyroid hormone (PTH) and active calcitriol, the active form of vitamin D. When PTH receptors in the DCT bind to PTH, Ca2+ is reabsorbed form the filtrate and back into the blood. Presence of calcitriol also induces the production of calcium-binding proteins, which help to transport Ca2+ into cells. Any calcium that is not reabsorbed at this point in the DCT will be excreted in urine- therefore in renal disease, where formation of calcitriol is impaired, more calcium will be excreted and patients may develop mineral bone disease (CKD-MBD- for more info on this, see my post on AKI and CKD).
ERYTHROPOIETIN PRODUCTION
EPO is a hormone produced by the kidneys that promotes formation of RBCs in the bone marrow in response to cellular hypoxia (which can be a result of anaemia, and therefore impaired oxygen transportation). EPO is produced by fibroblasts around the peritubular capillaries and PCT. Without EPO, there is a lack of erythropoiesis (formation of RBCs) which is why anaemia is so common in patients with CKD.
Renal function tests
Urine dipstick-

Bloods-

BONUS ROUND! Diuretics- mechanisms of action.
Different diuretics largely do the same thing- increase urine output by reducing reabsorption of water. But knowing where your diuretic will act is important to be able to work out what's actually going to happen when you give it, and avoid any unexpected effects...
Loop- work on the ascending limb of the loop of Henle and inhibit sodium reabsorption, which therefore inhibits water reabsorption. Examples include bumetanide and furosemide.
Osmotic- work on the PCT, distal DCT and collecting ducts. The drug is not reabsorbed and therefore increases osmolarity, and so carries water out with it. Examples include mannitol.
Thiazide- work on the proximal DCT.- specifically on the thiazide sensitive sodium-chloride co-transporters. By stopping sodium reabsorption, more water is excreted. Examples include bendroflumethiazide and indapamide.
Potassium sparing- work on the distal DCT and collecting ducts. Does what it says on the tin- stops you losing potassium in urine. Either act on sodium channels, or as aldosterone antagonists . Examples include amiloride and spironolactone.
Thank you for reading all the way through this post! I really hope you learnt something useful that you can take into practice with you. Below is a list of sources and resources, and I've bolded the ones that I think are most useful or that influenced most of this post!
Please like and comment on this post or on twitter/instagram (@christienursing) with any questions/suggestions, and feel free to share!
Love, Christie x
Sources...
Kidney Research UK (2006) 'Kidney Health Information: The Kidneys- a Basic Guide'. https://www.nhs.uk/Livewell/Kidneyhealth/Documents/kidney%20guide.pdf
Kidney Research UK (2008) 'Kidney Health Information- Protein in Urine (Proteinuria)'.
Lumen Learning- 'Chapter 14: The Urinary System and The Reproductive System- Physiology of Urine Formation'.
Lumen Learning- 'Urinary System- Physiology of the Kidneys'.
Khanna, A. (2020) 'Antidiuretic hormone'.
Willis, L. (ed) (2020) Fluid and Electrolytes Made Incredibly Easy!. 7th edn., pp. 297-311.
Marieb, E., Hoehn, K. (2016) Human Anatomy and Physiology. 10th edn.
This is easily my favourite resource for A+P. It's not the simplest in terms of langage and formatting, but it's comprehensive and gives you at least a reliable starting point from which you can go forth and google things
BC Campus Open Textbook. 'Anatomy and Physiology- Chapter 25-26 Tubular Reabsorption'.
Klabunde, R. (2016) 'Renin-Angiotensin-Aldosterone System'
Hsu, R., Hsu, C. (2016) 'The role of acute kidney injury in chronic kidney disease' in Seminars in Nephrology. 36(4), pp. 283-292. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4979984/
You and Your Hormones- 'Adrenal glands' https://www.yourhormones.info/glands/adrenal-glands/
Hansen, J. (2019) Netter's Anatomy Colouring Book. 2nd edn.
Scarth, E., Smith, S. (2016) Drugs in anaesthesia and intensive care. 5th edn.
Mather, A., Pollock, C. (2011) 'Glucose handling by the kidney' in Kidney International. 79(120), pp. 1-6
Wikipedia- 'Erythropoietin' https://en.wikipedia.org/wiki/Erythropoietin
Williams, S., Malatesta, K., Norris, K. (2009) 'Vitamin D and chronic kidney disease' in Ethnicity & Disease. 19(4), pp. 5-8. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2878736/